Factors affecting prevalence of neurological symptoms among workers at gasoline stations in Rayong Province, Thailand
Article information
Abstract
This cross-sectional study was aimed at assessing the exposure to organic solvents and the factors affecting prevalence of neurological symptoms among workers at gas stations in Rayong Province. The sample included 200 workers at gas stations, including refueling staff, cashiers, food shop, coffee shop, and convenience store employees. Interview questionnaire included general information, work history, and neurological symptoms. Urine collection devices were used to detect organic solvents metabolized in urine, including t,t-muconic acid (t,t-MA), hippulic acid (HA), mandelic acid (MA), and methylhppuric acid (MHA). The results showed that the workers’ medians (interquartile range: IQR) of the metabolized organic solvents were as follows: t,t-MA was 393.62 (244.59) μg/g Cr, HA was 0.32 (0.14) g/g Cr, MA was 0.06 (0.02) g/g Cr, and MHA was 0.40 (0.13) g/g Cr. For prevalence of neurological symptoms, top three symptoms were headache (49.0%), dizziness (42.5%), and stress/irritability (38.5%). Working at a gas station present was neurological symptoms more than in the past was 32.5%. According to the assessment of exposure to metabolized organic solvents and factors affecting the prevalence of neurological symptoms, overtime work ≥ 6 hours and HA content greater than quartiles Q3 had an effect on neurologic symptoms (OR=2.17; 95%CI=1.23–5.10 and OR=2.15; 95%CI=1.18–4.76, respectively). In summary, time spent working in gas stations and exposure to toluene organic solvents can cause neurological symptoms. It is recommended to reduce overtime or add breaks during work shifts or shift changes. In addition, workers should be away from the solvent.
Introduction
Thailand’s consumption of all types of fuels has had an increasing tendency. According to the statistics in 2019, the use of gasoline increased by 3.7% compared to the previous year. Gasohol was used the most, 97.0% of all gasoline groups, and the use of gasohol increased by 4.3% over the previous year [1]. Fuel consumption was much found in the major and economic provinces, one of which was Rayong Province, which has been developed as a province under the Eastern Economic Corridor project [2], with a large number of road transport businesses and regarded as an important tourist province in the eastern region of the country. A 2019 report indicated that gasoline consumption in Rayong Province was up to 5.7 hundred thousand liters per day [3], resulting in the expansion of gas stations to meet the demand. According to statistics from the Department of Business and Energy [4], Rayong Province had a total of 520 gas stations, which could be used as energy to develop the Thai economy over the past three decades.
The positive impact of the expansion of gas stations on the economy’s mobility is high. On the other hand, these gas stations are sources of release of organic solvents, especially BTEX (benzene, toluene, ethylbenzene, and xylene) [5]. Organic solvent vapors may be released from the refueling process, causing contamination in the atmosphere by 36.4% of various sources [6]. In the past, there was a study to assess the concentration of organic solvents in the atmosphere at gas stations in Iran. The mean benzene content during working was 2.01±0.41 μg/m3 [7], exceeding the occupational exposure limit (OEL) specified at 1.6 μg/m3 [8]. In Thailand, BTEX was surveyed at 7 gas stations. Benzene concentration was found to have a median of 114.4 ppb (minimum–maximum = 10.8–437.5) [9], which exceeds the REL-TWA (Recommended exposure limit - Time weighted average) specified at 100 ppb [10]. Toluene, ethylbenzene, and xylene concentrations were within the specified values.
As for the exposure to organic solvents of the BTEX group, upon entering the body, they will be rapidly distributed in the blood system and then metabolized by the Cytochrome P450-2E1 enzyme mainly in the liver, leading to the process of biotransformation to dissolve it in water and excrete it in the urine [11]. Therefore, biotransformation assessments are popular for practical assessments of individuals exposed to chemicals and organic solvents [12,13]. The American Conference of Government Industrial Hygienists (ACGIH) recommends an assessment of biomarkers of BTEX in the form of t, t-muconic acid (t,t-MA) [8], hippuric acid (HA) [14], mandelic acid (MA), and methylhippuric acid (MHA) [8] to assess the exposure to these substances.
Poisoning from exposure to organic solvents occurs in many systems, such as respiratory system, skin system [15], blood system [16], and nervous system [17]. However, as for the main health effects, there have been several reports of neurotoxicity of BTEX [17–20]. Gasoline metabolism process causes an oxidation stress, resulting in a neurotransmitter change or damage to bilayers and functions of sodium potassium adenosine triphosphatase [15] and thus leading to neurological symptoms [17]. According to Werder et al. [18], a one-quartile increase in BTEX exposure was 1.47 times the risk of developing neurological symptoms. In addition, there was a study in Khon Kaen Province, Thailand was detected air benzene reached an action level or higher than 50% of NIOSH REL (>50 ppb) and the workers had top three adverse symptoms, i.e., fatigue, headache and dizziness [20]. It can be seen that neurological symptoms are health conditions in which employees can perceive their change. Therefore, they may be used as a health screening parameter that can self-assess abnormalities. However, some reports suggest that the study of neurological symptoms should be monitored. If the exposure to fuel is less than 90 ppm, there may be no neurotoxic effect [15]. Other factors that may have an effect must also be controlled. Such as, near the sources of organic solvents in gas stations [21,22], gender [23], age [24], alcohol consumption [25,26], smoking [27,28], and personal protective equipment [29] etc. Therefore, these factors may influence neurological symptoms and should be investigated.
An assessment of health symptoms in people exposed to organic solvents is a guideline for preventing the severity of toxicity at an early stage while workers can observe the abnormal effects of organic solvents on their nervous system symptoms themselves. However, the past studies found these symptoms only in people who were exposed to high levels of benzene [12,15] or those in closed buildings in the industrial sectors [28]. The incidence of abnormal symptoms was unclear in those exposed to low concentrations of solvents [18,29,30], and no studies have been found among other workers at gas stations, such as those working in convenience stores, coffee shops, and food shops. In Thailand, there were only studies on refueling staff and cashiers [19,20,31]. Therefore, this study was aimed at assessing the exposure to organic solvents in urine and the factors affecting the prevalence of neurological symptoms among workers at gas stations in Rayong Province as a guideline for health screening for neurological disorders and for prevention of risk factors for these workers.
Materials and Methods
Study design and sample size determination
It was a cross-sectional study to collect information from a sample of workers at gas stations in Rayong Province. A sample of 200 people was calculated from a previous study of Chaiklieng and Nantanuch [19]. It was found that 83.7% of workers who had worked at gas stations experienced adverse symptoms (Proportion=0.837). The desired level of confidence was 95% (α=0.05), at a power of 95% (β=0.05). A cluster sampling was used until its completion because the working conditions of each gas station were similar. Inclusion criteria mainly focused on workers primarily working at gas stations, including refueling staff, cashiers, and food shop, convenience store, and coffee shop employees, for more than 3 months and agreeing to join the project voluntarily. Exclusion criteria included an illness on the sampling day or an exacerbation from their existing underlying diseases, such as migraine, allergy, and asthma, and an absence from work on the data collection day, respectively.
Ethics statement
This study was conducted in accordance with the Declaration of Helsinki. Burapha University Institutional Review Board for Protection of Human Subjects in Research (BUU-IRB) approved this research under certificate no. 019/2020.
Research tools
The present study used two types of research tools: interview form and urine collection devices and laboratory analyzer. The details of each tool are as below.
1. Interview form was divided into three sections includes general information, work history, and neurological symptoms: (1) general information includes gender, age, weight, height, smoking, alcohol drinking, and bed time per day; (2) work history includes work station area, work experience, working time per day, working period per week, personal hygiene, and wearing respiratory protective equipment; (3) neurological symptoms includes dizziness, headache, confusion, nausea/vomiting, fatigue/tiredness, drowsiness, less concentration/memory, stress/irritability, no/less smelling, changed tasting, hand/foot tip numbness, face numbness, arm/leg weakness, hand shaking, and less sexual sensation. fifteen neurological symptoms were mainly reviewed from the organic solvent neurotoxicity data of the National Institute for Occupational Safety and Health (NIOSH) [32]. In addition, the neurological symptoms from the previous studies [17,19,28] and reexamined for their association with organic solvents by the occupational medicine physicians.
For interview and interpretation of important variables, such as smoking factor, drinking alcohol factor, and workstation area as a disturbance variable affecting exposure to organic solvents and nervous system. For cigarette or tobacco smoking, the researcher interviewed the sample group. None of them smoked electronic cigarettes. The smoking variable was divided into two groups: (1) smokers are people who are currently smoking, or second-hand smokers are people who inhale tobacco smoke that is exhaled by smokers or given off by burning tobacco and inhaled by people nearby; (2) non-smokers are people who have never smoked and people who have given up or quit smoking cigarettes and/or tobacco. According to Kaukiainen’s research [33], the smoking groups were classified. This study looked at smoking and screening for neurological symptoms in workers exposed to organic solvents. When it came to drinking, alcohol was divided into two categories: (1) The drinking alcohol group includes all types of alcoholic beverages such as wine, beer, or distilled spirits, among others; (2) the non-drinkers group includes anyone who has never drank any alcoholic beverages or anyone who has stopped drinking alcohol [18]. Furthermore, the workstation area variable was divided into two groups based on their working area: (1) The working group at the fuel dispenser refers to those who work in the refueling gas service/cashiers; (2) the working group outside the fuel dispenser refers to those who work in the food shop/convenience store/coffee shop at gas stations [34].
As for the tool quality inspection, the interview form was assessed for the item-objective congruence index (IOC) by 3 experts comprising 2 occupational medicine physicians and 1 university professor in occupational health and safety. The IOC obtained was greater than 0.5 in all questions, which met the measurement and evaluation criteria.
2. Urine collection devices and laboratory analyzer included plastic glasses, 50 mL polyethylene pots, temperature-control foam boxes, ice packs, and high-performance liquid chromatography (HPLC). Criteria for interpreting the results were divided into 2 groups using the cut point: less than or equal to the Q3 and more than the Q3.
Tool quality inspection was conducted by a laboratory certified by the international quality control standard (ISO 15189: 2012) and the Thailand Ministry of Public Health (MOPH) standard. Metabolized organic solvents were analyzed according to the method of Onchoi et al. [33].
Data collection
Interview forms were collected by the researcher and research assistant who passed the training on interview items. On the sampling collection day, the interviews were conducted around the gas stations prepared by their owners. Data collection was conducted after the end of work and took about 15–20 minutes to interview each person, after which the interview forms were checked.
Urine sample collection was conducted by the researcher. Initially, the researcher clarified the urine sample collection that was conducted at the end of the work shifts. Mid-stream urines were collected into a plastic cup and then poured into a polyethylene pot of at least 50 mL or about half a urine pot. After that, the urine samples were immersed in a foam box at the temperature below 4 °C and taken to the laboratory for analysis on the same day the samples were collected for analytical testing for metabolized organic solvents, including t,t-muconic acid (t,t-MA), hippuric acid (HA), mandalic acid (MA), and methylhippuric acid (MHA).
Data analysis
The analysis was done by descriptive and inferential statistics according to the measurement level of the variables. Discrete variables, such as gender, smoking, and alcohol drinking, were analyzed by frequency and percentage. Continuous variables were tested for the data distribution by the Kolmogorov-Smirnov test. Normally distributed data were described by means and standard deviations, while abnormally distributed data were described by geometric mean (GM), geometric standard deviations (GSD), medians, interquartile ranges (IQR), minimum, maximum and quartiles. The grouping of metabolized organic solvents used the Q3-based cut point.
Inferential statistics were used to compare neurological symptoms occurring in the present (T1) and before coming to work at this gas station (T2) as well as to calculate the number change from the formula (T1–T2), and McNemar test used comparing symptoms between present and past in same person. The association between the general information, work history factors and the overall prevalence of neurological symptoms was analyzed by univariate analysis indicate crude odds. Factors with a significant (p-value of less than 0.05) from univariate analysis were selected to analyzed with organic solvents metabolites by multiple logistic regression. Several combine factors, such as t,t-MA, MHA, MA, HA, and working overtime were adjusted to indicate adjusted odds and 95% CI.
Results
General information and work history
According to the study of general information of (n=200), about two-thirds were female, aged over 30 at 57.0%, and body mass index with overweight or obese at 56.0%. In addition, most of the workers earned more than 305 USD (10,000 baht) per month at 56.5%, about one-thirds had smoking behavior, and workers had alcohol drinking behavior at 45.5%. When comparing general information factors and gender, males were statistically significantly more overweight, smoking, and consuming alcohol than females.
As for the work history of workers, most of them were employed for more than 1 year at 73.5%, work time less than or equal to 8 hours at 54.0%, working every day at 55.5%, weekly overtime more than six hours at 86.5%, and most had good hygiene practices and used personal protective masks at 79.0% and 69.5%, respectively. When comparing work history factors and gender, males had statistically significantly more work hours per day and worked every day than females. However, females statistically significantly more worked in buildings, such as food and coffee shops and convenience stores, than males Table 1.
Exposure to metabolized organic solvents
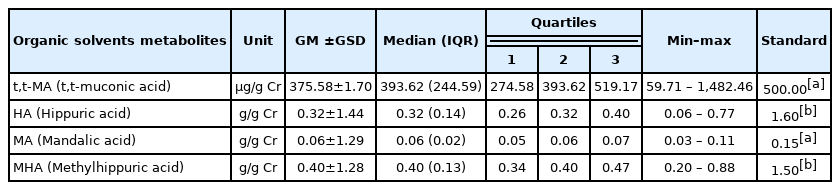
From the study of exposure to organic solvents metabolites, workers had t,t-MA content after work exceeding the ACGIH recommendation at 29.5%, with the highest value of 1,482.46 μg/g Cr. However, for HA, MA, and MHA in their urine, all parameters met the standard criteria Table 2.
Comparison of the prevalence of neurological symptoms occurring in the present and past before working at this gas station
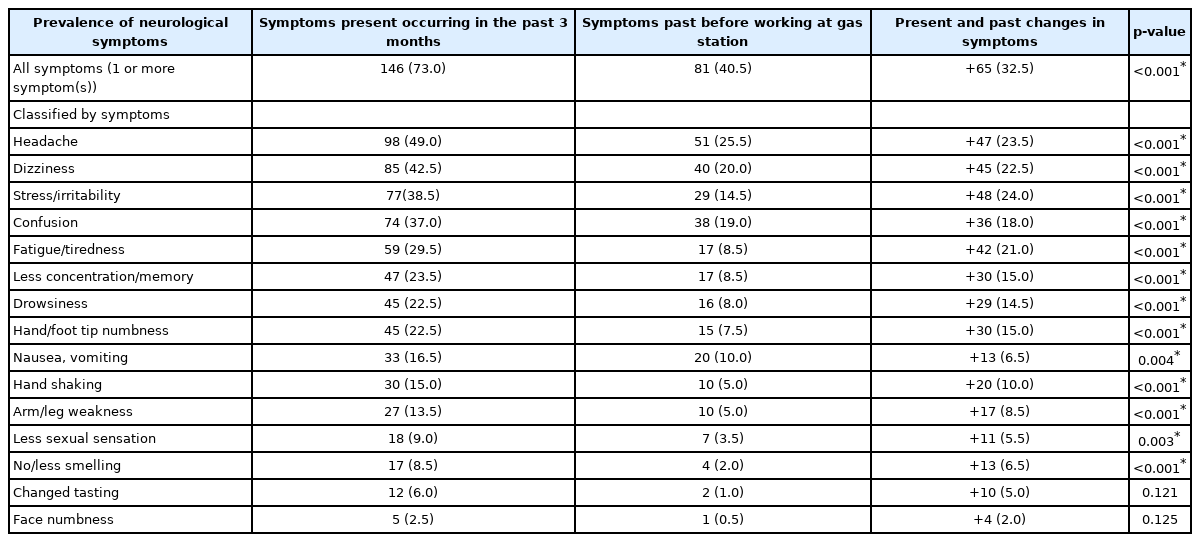
Overall neurological symptoms interviews revealed that at present workers had one or more neurological symptoms at 73.0%. In contrast, before coming to work at this gas station, they had these symptoms at 40.5%, which was an increase of 32.5%. When classified by individual symptom, at present workers had headache the most, followed by dizziness and stress/irritability at 49.0%, 42.5%, and 38.5%, respectively. While other neurological symptoms are shown in the Table 3.
Exposure to metabolized organic solvents and factors affecting the prevalence of neurological symptoms
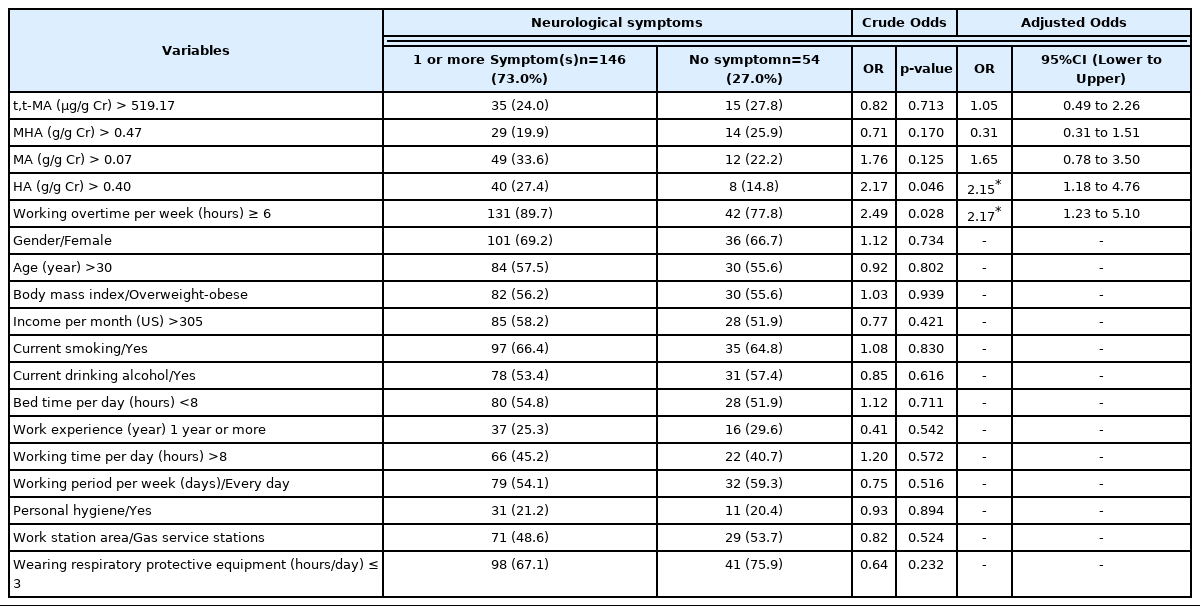
According to the study of factors, including general information, work history, and exposure to metabolized organic solvents and neurological symptoms as a whole, working overtime more than or equal to 6 hours was 2.17 times the risk of neurological symptoms (95%CI=1.23–5.10) and HA content in urine was greater than the Q3 (greater than 0.40 g/g Cr) with 2.15 times the risk of neurological symptoms (95%CI=1.18–4.76). For other factors, no correlation was found Table 4.
Discussion
The study evaluated the exposure to metabolized organic solvents. Workers had t,t-MA content, metabolized benzene, after work the most at 1,482.46 μg/g Cr, there were 59 out of 200 workers ( 29.5%) above the standard concentration (500 μg/g Cr) specified by the ACGIH [8]. This can be seen that benzene is still a problem at gas stations. As evidenced by a study in Iran measuring BTEX in the environment at gas stations, benzene concentrations exceeded the OEL threshold [7]. However, in this study, urinary metabolites were assessed and the results of the study were similar to those in Brazil where urinary metabolites were assessed and the mean at 95th percentile of t,t-MA among the refueling staff was 785 μg/g Cr, which was 2 times greater than those in the control group [34]. Contrarily, this study assessed the exposure to other chemicals, i.e. HA, MA, and MHA, in urine. All workers had these metabolized organic solvents not exceeding the ACGIH standards. This study points out that benzene is still a more problematic chemical that should be monitored for exposure than any other chemicals among gas station workers.
Neurological symptoms were the main symptoms associated with exposure to organic solvents in the BTEX group. In this study, the interviews were conducted regarding the present symptoms occurring within 3 months and before working at gas stations. The data collection design differed from several studies [12,19,34]. Most studies inquired workers after their work only. This study collected information to confirm the causes from working at gas stations. From the results analysis, an interesting point was that at present the worker had more neurological symptoms than in the past before working at this gas station with a statistical significance (p<0.05) for a total of 13 symptoms (from 15 symptoms interviewed), including dizziness, headache, confusion, nausea/vomiting, fatigue/tiredness, drowsiness, less concentration/memory, stress/irritability, hand/foot tip numbness, arm/leg weakness, hand shaking, less sexual sensation, and no/less smelling. The first 3 symptoms mostly found were headaches, dizziness, and stress/irritability at 49.0%, 42.5%, and 38.5%, respectively. The results of this study confirmed that working in a gas station resulted in an increase in adverse neurological symptoms. Operations near the sources of organic solvents in gas stations were therefore likely to be exposed to fuel vapors [22,34]. The results were also consistent with the previous study by Werder et al. [18] who found that the sample exposed to organic solvents had at least one neurological symptom at 49.0%, any of which was a central nervous system symptom at 32.0% while the most common symptoms were headache and dizziness. Additionally, according to a Thai study by Chaiklieng and Praengkrathok [37], refueling workers experienced headache/confusion/fatigue at 68.7%. Similarly, several studies suggested headache as a predominant symptom due to the exposure to organic solvents [19,29,38] since organic solvents have a mechanism capable of passing through the blood brain barrier as well as of depressing and interfering with neurotransmitter functions [39]. Evidence of brain abnormalities was reported on magnetic resonance imaging (MRI) tests in patients with exposure to substances in fuel for 18 months [15] and is therefore academic data supporting the linkage of organic solvents and neurological symptoms.
As for the working overtime per week factor, the results of this study indicated that overtime more than or equal to 6 hours had an effect on neurological symptoms (OR=2.17; 95% CI=1.23–5.10). More than half of the workers worked every day at 55.5% and most of them worked overtime more than 6 hours per week at 86.5%. The work station area at gas stations is diverse, including both formal and informal workers, such as workers responsible for refueling, food shop, and convenience store services. Refueling workers work in shifts, about 8 hours each. During their shift change, if there are still many customers, they will have to work about 1–2 hours overtime to keep up with customer services. In addition, food shops in gas stations must be open to meet consumers in the morning, noon, and evening. Therefore, in this study, workers had more work hours than those in factories. Considering legal requirements prescribing the periods of work that can be dangerous to the health and safety of employees who must work no more than 8 hours per day or 48 hours per week [40], it can be seen that workers at gas stations work longer than those required by law; therefore, they are more likely to be exposed to chemicals in fuel for a long time, resulting in health effects.
Moreover, the results on working overtime per week factor were consistent with Chaiklieng and Praengkrathok [37] reporting that workers serving at urban and suburban gas stations had average working hours of 8.60 and 9.79 hours per day, respectively. This study also found that working at gas stations in the present resulted in a higher risk of neurological disorders than in the past before coming to work. If the work time at gas station increased, the risk of neurological symptoms was higher. These findings are therefore academic data showing that the longer duration of exposure to chemical threats in the gas stations can cause effects on the nervous system. This is consistent with several studies on durations of work in relation to the central nervous system (CNS) and the peripheral nervous system (PNS) [41,42]. For example, according to Mandiracioglu et al. [28], working hours of more than 8 hours per day were associated with increased blood toluene and benzene levels, resulting in loss of reflexes. Even at low-exposure gas stations and working outdoors, they could have neurotoxic effects.
As for the urinary BTEX content, another point found was that although the content of HA in the urine (metabolized toluene) did not exceed the standard, workers had more HA than the Q3 along with 2.15 times more likely to develop neurological symptoms (OR=2.15; 95% CI=1.18–4.76) than those exposed less than the Q3. This is consistent with previous studied in both animals and humans. For example, from a study with 20 rabbits, the experimental group received toluene at a 99.9% solution concentration intraperitoneally at a dose of 876 mg/kg. In this experimental group, there were biochemical associated with neurotransmitters, i.e. dopamine, nerve growth factor (NGF), and glial fibrillary acidic protein (GFAP), which were statistically significantly lower than those in the control group (p<0.05). These are brain activity indicators, such as NGF developed from hippocampal neurons [43]. In addition, a human study in Iran examined airborne BTEX with systemic symptoms and found that airborne toluene content was found to be most positively associated with neurologic symptoms with a statistical significance (r=0.577, p<0.001) [17]. Although both studies used different toluene assessment tools from this study, namely, studies in Iran used atmospheric measurements of BTEX at gas stations, this study assessed exposure by measuring BTEX as metabolized urine, but the results of the studies were consistent.
In addition, the present study did not find a correlation between the content of t,t-MA, MHA, and MA in urine and the prevalence of neurological symptoms, possibly because the manifestation of neurological symptoms was associated with different dose-dependent responses to BTEX for each substance. For example, the ATSDR [44] report states that an airborne dose of benzene greater than 210 ppm can cause acute neurotoxic effects. However, this study was a long-term exposure to low concentration substances. Moreover, this study was consistent with research in a similar context among refueling workers in Bangkok, Thailand. It was found that benzene was not associated with neurological symptoms [30]. A study in Izmir, suggested that the benzene exposure group and the control group had no difference in scores of neurological symptoms [28].
However, from this exposure assessment, approximately one-third of workers had higher t,t-MA content than the standard. Therefore, health surveillance in high-risk groups should be monitored in terms of the effects on the body from exposure to this type of BTEX. Previously, benzene was said to be a blood-sensitive toxicity [15] and a carcinogen [45]. With a surveillance of neurological symptoms, the exact dose of exposure of the substances that affect neurological symptoms may thus not be known. Therefore, there should be a further study and surveillance of BTEX in the body and neurological symptoms.
In this study, there was no correlation found between the general information factors, such as gender, age, smoking behavior, and alcohol consumption, and the neurological symptoms, which was different from previous studies. For example, age factor, it was reported that employees over 30 years of age had more symptoms of central nervous system (CNS) disorders than those under the age of 30 years with statistical significance (the prevalence of CNS symptoms was 63.1% and 22.6 percent, respectively) [24]. For health behaviors, such as alcohol consumption among workers exposed to organic solvents, those who regularly or occasionally drank alcohols had more neurological symptoms than non-drinkers [25,26]. For smoking [27,28], it affected the response of autoimmunity system, caused the inflammation, and increased the risk of multiple sclerosis [29]. It might be possible that the samples had homogenous data due to their similar age and year of work, etc. In addition, as the rules of operations at gas service stations strictly prohibit employees from smoking in their work areas due to the flammable substances, the frequency of smoking is limited. Therefore, the chemicals in cigarettes may not be exposed enough to cause neurotoxic effects. This was unlike previous studies where factory workers working in buildings with greater autonomy of behavior and diversity of demographic characteristics than this study were investigated. However, the confounding factors of this study were considered controlled, which primarily wanted to assess the BTEX exposure and its effects on the nervous system. Furthermore, neurological symptoms may be caused by factors other than work, such as lifestyle or physical activity. There have been reports in the past of a lack of physical activity affecting the risk of brain development. Exercise and physical activity, on the other hand, have anti-inflammatory effects throughout the body [46]. As a result, exercise may help to relieve neurological symptoms. Future research should take into account factors outside of the workplace.
The highlight of the study was that the researcher interviewed the past neurological symptoms before working at gas stations as well as interviewed the current symptoms in the same workers. It was considered as a control over various confounding factors, such as personal factors or individual behaviors. This resulted in the reliability of symptom outcomes. In addition, the number of samples was more sufficient to answer the research objectives than many previous studies on the same issue. However, the limitation of this study was that data collection was conducted during the first wave of the COVID-19 outbreak in Thailand, which might result in lower fuel consumption than normal.
Conclusions
The conclusion of the study could confirm that working at gas stations has a greater effect on neurological symptoms. In health screening, 13 neurological symptoms can be used as a guideline. In addition, factors contributing to neurological symptoms were overtime and exposure to toluene. Although toluene content was found not exceeding the standard, it could cause neurological symptoms. However, further studies in the future should investigate the exposure dose for each substance that is particularly sensitive and specific to neurological symptoms or analyze the combined organic solvent mixtures because there are many substances in the fuel that affect the nervous system.
Acknowledgement
We express our gratitude to the Public Health System Research Institute for funding this research (Contract No. 63-070). This work was supported by Burapha University. We thank the staff of Rayong Hospital in honor of Her Royal Highness Princess Maha Chakri Sirindhorn for allowing us to collect samples. We are grateful for the participate.
Notes
No potential conflict of interest relevant to this article was reported.
CRediT author statement
CPP: Conceptualization, Methodology, Investigation, Resources, Formal analysis, Data curation, Writing-Original draft Preparation; AT: Conceptualization, Methodology, Writing-Review & Editing, Project administration, Funding acquisition.