AbstractMercury chloride (HgCl2) is a neurotoxicant that remains a health hazard despite numerous efforts to reduce its levels in the environment. The use of medicinal plants in treating various diseases and other toxic agents has grown popular owing to their effectiveness and affordable rates. Andrographis paniculata (A. paniculata) is a plant with astringent and detoxifying characteristics and is widely used worldwide for its medicinal and antioxidant benefits. This study aimed to investigate the possible protective effects of A. paniculata aqueous extract against HgCl2-induced memory impairment, oxidative stress, and brain damage. Twenty-five adult Wistar rats were randomly divided into five groups: control, HgCl2 0.5 mg/kg, HgCl2+AP 250 mg/kg, HgCl2+AP 500 mg/kg, or HgCl2+Ascorbic acid 200 mg/kg. For 28 days, administrations were given through oral gavage once a day. HgCl2 injection resulted in memory impairment, increased glutamate concentrations in the brain, and the production of oxidative stress. Memory impairment was prevented in A. paniculata-treated groups by balancing the levels of AChE and dopamine activities, which then lowered glutamate concentration, avoided oxidative stress, and improved histopathological alterations in the brain. A. paniculata alleviated HgCl2-induced memory impairment in Wistar rats by increasing the memory index, regulating neurotransmitter levels, and reducing oxidative stress.
IntroductionHeavy metals such as mercury, lead, and nickel accumulate in air, water, and land due to increased industries resulting from development [1]. Mercury (Hg) exposure has increased globally due to industrial activities, gold mining, medicinal uses, and fossil fuel combustion [2]. Occupational mercury chloride (HgCl2) exposure resulted in neurotoxicity, including cognitive impairment, motor dysfunction, central auditory system dysfunction, nephrotoxicity, hepatotoxicity, and mortality [3]. It primarily damage brain tissue, causing focal brain damage that can affect the function of brain parts like the cerebellum, hippocampus, and visual cortex and cause cognitive and behavioral changes [4]. Many investigations have shown that mercury causes toxicity by producing reactive oxygen species (ROS) and rapidly depleting beneficial antioxidant enzymes such as catalase, superoxide dismutase (SOD), and glutathione peroxidase (GSP). ROS promotes mitochondrial malfunction, neuroinflammation, and apoptosis, all of which contribute to neurodegenerative diseases and neuronal cell death [5]. Mercury accumulation in brain tissue increases the expression and reactivity of N-methyl-D-aspartate (NMDA) receptors. Activation of NMDA type glutamate receptors enhances Ca2+ entry into neurons, which motivates neuronal cell death pathways. Furthermore, Ca2+ promotes ROS production via the mitochondrial pathway [6,7].
The hippocampus is responsible for integrating two forms of memory: event storage and recall. The biochemical activities proceed along neuronal transmission channels, with the hippocampus playing a critical role in cognitive and behavioral analyses [8]. Previous investigations in the hippocampus confirmed the existence of elevated amounts of Hg in the brain parenchyma following prolonged exposure to HgCl2 [9] and compromised its crucial role in learning and memory [10]. Despite HgCl2’s limited capacity to penetrate biological barriers, it can nevertheless result in motor impairments because it induces apoptosis and reduces the number of neurons and astrocytes in the motor cortex [11].
Despite drug development research, treatment for neurological disorders remains abysmal due to modern drugs’ failure to regenerate central nervous tissues and their adverse side effects. Because oxidative stress is a common occurrence in metal toxicity, it is critical to comprehend the interaction between antioxidants and neurotoxicants like HgCl2. The antioxidant activity of medicinal plants is primarily responsible for the benefits associated with antioxidant consumption [12].
A. paniculata is a medicinal plant with much potential for treating various diseases [13]. A. paniculata contains a variety of compounds, including labdane diterpenoid lactones, flavonoids, and other compounds. It has a diverse set of pharmacological properties that have been demonstrated [14]. In Asia, America, and Africa, the plant has been used to treat various illnesses [15]. The Indian Pharmacopoeia includes this plant and is used in approximately 26 Ayurvedic formulations [16,17]. Andrographolide is the main medicinal component of A. paniculata [18]. Antioxidant, antimicrobial, anti-inflammatory, and antihyperglycemic properties are also found in A. paniculata [19]. Andrographolides are quickly excreted from the body through the urine and digestive tract. A. paniculata is an ideal substance for treating and preventing many ailments due to its wide distribution to the organs and regulatory actions [20]. Antioxidant-rich herbal plants protect against oxidative stress-related diseases such as neurodegenerative disease, cancer, inflammation, and cardiovascular disease [21]. This study examines whether A. paniculata could protect rats from HgCl2-induced memory loss by assessing acetylcholinesterase, neurotransmitter concentrations, and oxidative stress. In addition, the study assessed the histology and histochemistry of the rats’ hippocampus and cerebellum.
Materials and MethodsMercury chloride, (BDH Chemicals Ltd, England) was used as neuronal toxicant. Vitamin C (Ascorbic acid; 70 mg/tablet) produced by Micro Labs Limited with NAFDAC number A4-6344, was obtained from a reputable pharmaceutical store (M.U.B Pharmaceutical Enterprises Ltd.) Zaria, Kaduna state, used as standard drug for Antioxidant. Ketamin (Sigma-Aldrich Co. LLC St. Louis, USA), Phosphate Bufffer Saline (PBS), 70% Ethanol (Sigma-Aldrich Co. LLC St. Louis, USA), Distill Water, measuring cylinders and beakers.
Plants collection and authentication
A. paniculata aerial pieces were obtained from Idoani, Ose Local Government Area, Ondo State. The plant specimen was identified and certified in the herbarium division of Ahmadu Bello University’s Department of Botany in Zaria, and voucher number 1331 was issued for reference.
ExtractionThe A. paniculata plants were air dried at room temperature to a consistent weight and pulverized with a pestle and mortar. 500 g of dry plant material was macerated in 5 L of distilled water for 48 hours. The aqueous extract was filtered using Whatman filter paper, and the mixture was evaporated till dry using a controlled hot water bath maintained at 60–70 °C. The dried A. paniculata seed extract was stored in a 4 °C refrigerator until use. The extract was given to the rats in the form of daily suspensions in distilled water [22].
Experimental animalsTwenty-five male and female Wistar rats were obtained from the Animal House, Department of Pharmacology, Faculty of Pharmaceutical Sciences, Ahmadu Bello University, Zaria, and fed commercial grower mash feed with free access to water. The animals were housed in clean iron cages with twice-weekly bedding changes. They were acclimatized for ten days, and the rats were cared for following internationally recognized animal welfare standards. With Approval No: ABUCAUCC/2020/22, the Ahmadu Bello University Committee on Animal Use and Care (ABUCAUC) granted ethical approval.
Experimental procedureThe rats were randomly divided into five groups (n=5). The administration of mercury chloride, ascorbic acid, and A. paniculata aqueous extract is summarized in Table 1. The dose of HgCl2 (0.5 mg/kg) used in this experiment is an equivalent dose that has been linked to organ toxicity as previously reported [23]. The HgCl2 was administered via intraperitoneal injection, whereas the A. paniculata and ascorbic acid were administered via oral gavage. The experimental animals were weighed weekly before and during the study. The treatment period lasted 29 days.
Procedure for samplingRats were slaughtered humanely at the end of the experiment while under ketamine anaesthesia (75 mg/kg intraperitoneally). Wistar rat brain tissues were acquired and placed on ice in a Petri plate (24,25). Brain tissue was, washed in ice-cold saline, and homogenized in Phosphate Buffer Saline (pH 7.4) using a Teflon homogenizer. The brain homogenate was centrifuged at 5,000×g to eliminate cellular debris. The supernatant of the obtained brain homogenates was stored at −20 °C until use.
Assay for biochemical parametersThe supernatants were used to estimate biochemical markers such as superoxide dismutase activity (SOD), catalase activity (CAT), malondialdehyde (MDA), acetylcholinesterase, glutamate, and dopamine.
Assay of lipid peroxidationMalondialdehyde (MDA) concentration is one of several low molecular weight end-products of lipid hydroperoxide breakdown and is used as a lipid peroxidation indicator. The production of TBARS, as assessed by the modified technique of Niehaus and Samuelson [24] and described by Akanji et al. [25] indicates lipid peroxidation. The 150 l of serum homogenate were treated with 2 mL of TBA-TCA-HCL reagent (1:1:1 ratio) and placed in a water bath at 90 °C for 60 minutes, then cooled and centrifuged at 5000 rpm for 5 minutes, and the absorbance of the pink supernatant (TBA-Malonaldehyde complex) was measured at 535 nm. The molar extinction coefficient of 1.56×10−5 cm−1M−1 was then used to compute the amount of malonaldehyde produced.
Assay of catalase (CAT) activityCatalase (CAT) activity was determined using Aebi’s technique [26]. 100 μL of serum was added to a test tube containing 2.80 mL of 50 mM potassium phosphate buffer (pH 7.0). To initiate the reaction, 1 mL of newly prepared 30 mM H2O2 was added to start the reaction, and the rate at which it decomposed was measured using a spectrophotometer for 5 minutes at 240 nm. The catalase activity was calculated using a molar extinction value (E) of 0.041 mM−1-cm−1. One unit was the quantity of catalase that decomposes 1 μmol of H2O2 per minute at pH 7.0.
Assay of superoxide dismutase (SOD) activityFridovich’s [27] technique for determining superoxide dismutase (SOD) was used. This assay is based on the ability of superoxide dismutase (SOD) to inhibit auto oxidation of adrenaline at pH 10.2. To produce a 1:10 dilution of microsomes, 0.1 mL of serum was diluted in 0.9 mL of distilled water. A 0.2 mL aliquot of the diluted microsome was mixed with 2.5 mL of 0.05 M carbonate buffer. The reaction was initiated by adding 0.3 mL of 0.3 mM adrenaline. 2.5mL of 0.05 M carbonate buffer, 0.3 mL of 0.3 mM adrenaline, and 0.2 mL of distilled water comprised the reference combination. The absorbance was measured at 480 nm for 30 seconds to 150 seconds.
Assay of glutathione peroxidase (GPx)GPx activity was assessed using Paglia and Valentine’s [28] technique with H2O2 as the substrate. The rate of NADPH oxidation at 240 nm over the course of three minutes served as an indirect indicator of the process. When hydrogen peroxide was added to a 0.1 M Tris buffer solution with a pH of 8.0, a blank without homogenate was used as a control. The measure of enzyme activity was nmol/mg protein.
Assay of acetylcholinesterase enzymes, glutamate and dopamineAn enzyme-linked immunosorbent assay (ELISA) kit was used to assess the levels of acetylcholinesterase enzymes, glutamate and Dopamine according to the manufacturer’s instructions (ACON Labs, USA).
Histological and histochemical studiesThe brain was dissected out, the hippocampus and cerebellum were carefully excised, and the tissue was post-fixed in neutral buffer formalin for 24 hours before processing for histological staining. The tissues were dewaxed in two changes of xylene for three minutes each, then hydrated for three minutes each in decreasing grades of alcohol (100%, 95%, 90%, and 70%) before being rinsed in tap water to remove excess stain. The slides were then once again rinsed with tap water after being briefly submerged in acid alcohol for distinction. Scott’s tap water was used to blue the slides for 5 minutes, after which they were counter stained with Eosin for 3 minutes. After being washed in tap water, the sections were dehydrated in successively stronger alcohols and then cleaned in xylene. After that, a mountant was used to cover-slip the parts for general histology [29].
Bielschowsky silver stainingSections that had been deparaffinized and rehydrated were then incubated in a 20% silver nitrate solution for 25 minutes at pre-warmed (37 °C), rinsed three times with distilled water, and then submerged in 10% formalin to halt the silver reaction. Then, drop by drop, ammonium silver solution was poured onto the slides, and after washing with 10% formalin, the sections were allowed to dry until they were a deep brown color. They were then rinsed with distilled water for 5 minutes, deposited in a 5% sodium thiosulfate solution for 5 minutes, dehydrated, hyalinized, and mounted [30]. After that, the tissue samples were examined and photographed using a light microscope (Olympus CHNB107MVR, Tokyo, Japan) to look for structural abnormalities at a magnification of X 250.
ResultsEffects of the extract on the weight gain of the experiment ratsRats treated with HgCl2 significantly reduced weight gain (p<0.05) when compared to controls, but rats treated with A. paniculata and HgCl2 had a significant weight gain in a dose-dependent manner. No significant difference (p>0.05) between the rats treated with the low dose of A. paniculate and the rats treated with only HgCl2 (Table 2).
Oxidative stress biomarkersThe study’s findings revealed a substantial decrease (p<0.05) in SOD, CAT, and GPx concentrations in HgCl2 treated rats as compared with control rats and rats treated with A. paniculata (250, and 500 mg/kg+HgCl2) (Figure 1A, B and C). In the case of MDA oxidative stress indicators, HgCl2 treated rats showed a significant increase (p<0.05) compared with rats treated with A. paniculate. (Figure 1D).
NeurotransmittersShows the effect of mercury chloride and A. paniculata extract on Acetylcholinesterase, Dopamine, and Glutamate level. The results of the study showed a significant decrease (p≤0.05) in Acetylcholinesterase and Dopamine in HgCl2 treated rats compared with the control rats and rats treated with A. paniculata (250 and 500 mg/kg)+HgCl2, respectively (Figure 2A and B). The rats treated with A. paniculata of 500 mg/kg showed a more protective role in ameliorating the effect of HgCl2. While for the Glutamate, a significant increase (p<0.05) was observed in HgCl2 treated rats compared with the other experimental groups. No significant difference (p>0.05) was observed in all treated rat’s groups (Figure 2C).
Histological evaluationThe architecture of the Hippocampus, the control’s CA1 and CA3 sections revealed densely packed, linearly oriented pyramidal cells with a well-defined form. (Figure 3A). The HgCl2-treated group, on the other hand, showed architectural deformation, particularly in the pyramidal layer, as well as cell loss and cellular disarray; the group also had cytoplasmic characteristics suggestive of cell death (Figure 3B). Compared to the control group, distortions were drastically reduced in the HgCl2+AP250 mg, HgCl2+AP 500 mg, and HgCl2+AA groups. These groups had identical cell arrangements with an intact nucleus and well-defined borders, with sporadic patches containing few, haphazardly distributed cells displaying minor reactive neurodegenerative alterations such as necrosis and certain degrees of neuronal loss (Figure 3 C, D and E). The bielschowsky stain revealed normal neuronal organization and well-organized neuronal processes (Figure 4).
In contrast, HgCl2-treated rats showed architectural deformation and neural process degeneration (Figure 4). When HgCl2+AP 250 mg, HgCl2+AD 500 mg, and HgCl2+AA treated rats were compared to the control group, mild distortion and loss of neuronal processes were seen in the CA1 area (Figure 4). In contrast, rats treated with only HgCl2 showed marked degeneration and neuronal death in the CA3. The cytoarchitecture of the molecular, granular, and purkinje cell layers seemed normal in the cerebellar control rats (Figure 5B). Rats treated with just HgCl2 exhibited a standard molecular layer with Purkinje cell layer degeneration and Purkinje cell layer degeneration, whereas the granular layer showed aberrant packed granular cells (Figure 5B). Rats given A. paniculata (250 mg/kg) had severely deteriorated Purkinje cells with the Purkinje cells, but rats given A. paniculata (500 mg/kg) had distinct molecular and granular layers, with minor degeneration of the Purkinje cells inside the Purkinje cell layer and an average orientation of the molecular layer (Figure 5D and E).
DiscussionIn this study, animals given HgCl2 had a decreased gain in body weight. This result is consistent with what other researchers have observed [31,32]. The main sign of Hg toxicity is weight loss, which has been linked to decreased food consumption and rat muscle cell damage [33,34]. A. paniculata administration in this study was able to prevent such a side effect. The extract appears to have the potential to increase appetite and protect cells from oxidative stress caused by mercury, as a result, the rats’ weight improved [35]. One of the immediate effects of HgCl2 toxicity and poisoning in living organisms might be changes in oxidative state, either through excess generation of oxidants or deficiencies in antioxidant activity [4]. The current study discovered an increase in MDA and a decrease in SOD, CAT, and GPx levels in the brain tissues of HgCl2-induced rats. Regardless of the dose used, A.paniculata treatment did, however, attenuate these changes. These findings were consistent with prior research that found A.paniculata to have antioxidant effects [36–38]. The presence of bioactive compounds such as flavonoids and phenols in A. paniculata may be responsible for the antioxidant effect. Flavonoids have antioxidant properties by scavenging free radicals, preventing lipid peroxidation and playing a neuroprotective role in these studies [39]. A. paniculata has been shown to help with antioxidant defenses in previous studies [40,41]. It works by mitigating the free radicals directly. It indirectly affects mitochondrial integrity by inhibiting pro-oxidant enzymes and activating antioxidant enzymes. It can also activate enzymatic and non-enzymatic antioxidants, primarily through the Nrf2 signaling pathway [42].
Long-term exposure to HgCl2 causes neurotoxicity [43], affecting neurotransmitter synthesis and release [44]. In this current study, HgCl2 appears to reduce DA and AChE activity. A decrease in AChE and DA has also been linked to increased lipid peroxidation [45]. Previous research in rodents and humans has found a strong link between an age-related decrease in AChE, DA and increased oxidative stress. AChE activity is reduced by free radicals and increased oxidative stress [46,47]. However, the toxic and harmful effects of HgCl2 on AChE and DA activity were prevented by A. paniculata administration. A. paniculata promotes AChE activity even with HgCl2 exposure, which could be due to its ability to inhibit Hg-induced ROS and lipid peroxidation.
In the CNS, the excitatory neurotransmitter glutamate is the most abundant and is involved in neuronal plasticity, differentiation, and transmission [48]. On the other hand, excess glutamate causes abnormal depolarization of neurons, which causes excitotoxicity and death of neuronal cells [49]. The significant increase in glutamate concentration in HgCl2-treated rats may be due to the fact that HgCl2 can inhibit glutamate uptake by astrocytes at the synaptic space while stimulating glutamate release, resulting in excessive glutamate accumulation in the CNS’s extracellular space [50]. Notably, in this study, A. paniculata modulated glutamate concentration in HgCl2-treated rats. Furthermore, A. Paniculata might be able to regulate the glutamate concentration by increasing cellular uptake of glutamate to keep extracellular glutamate levels low. A. paniculata’s antioxidant potential may help prevent depolarization of cell membranes by regulating glutamate levels and preventing excitotoxicity just like other plant antioxidant potentials, as stated in a previous study [51].
Rats treated with just HgCl2 revealed neuronal degeneration, with shrunken nuclei and vacuolated cytoplasm, and some neurons with pyknotic nuclei or karyolysis at the CA1 and CA3 areas of the hippocampus, which is consistent with previous findings [52]. The degeneration of Purkinje cells within the cerebellum of rats treated with just HgCl2 showed the complete loss of nuclear materials, demonstrating the toxicity of HgCl2 [53,54]. However, treatment with A. paniculata prevented the above-mentioned HgCl2-induced morphological aberrations in the rats. The results obtained from this study are in accordance with the results documented in previous studies on the attenuating effects of Antioxidant rich plant on heavy metal-induced neurotoxicity [53]. These suggest that A. paniculata has antioxidant properties, as seen in the present study, or a combined antioxidant and anti-inflammatory role by Andrographolide, one of the major chemical constituents of the plant A. paniculate could be attributed to these positive preventive properties [40,55].
ConclusionsThis research reveals that HgCl2 (0.5 mg/kg) causes an oxidative imbalance in rat’s brain tissues, resulting in oxidative stress and pathological damage. HgCl2 produced toxicity in the hippocampus and cerebellar tissues and was effectively prevented by oral A. paniculata extract therapy at a dosage of 500 mg/kg/day. As a result, we conclude that A. paniculata extract might be effective as a potential protective/preventive agent in brain tissue damage caused by HgCl2 poisoning.
AcknowledgementMr Jigo Yaro, Chief Medical Laboratory Scientist, Department of Pathology, Ahmadu Bello University Teaching Hospital, and Mr Ayegbusi Olu, Department of Chemical Pathology, deserve special recognition for taking the time to run the biochemical assay and process the tissues.
NotesCRediT author statement
ESO: Conceptualization, Methodology, Validation, Formal Analysis, Investigation, Resources, Writing - Review & Editing; WM: Methodology, Formal Analysis, Investigation, Visualization, Writing - Original draft Preparation; AYS: Methodology, Formal Analysis, Investigation, Data Curation; SAB: Formal Analysis, Investigation, Visualization; AA: Formal Analysis, Investigation; RH: Visualization, Writing-Reviewing and Editing.
References1. Ijomone OM, Okori SO, Ijomone OK, Ebokaiwe AP. Sub-acute nickel exposure impairs behavior, alters neuronal microarchitecture, and induces oxidative stress in rats’ brain. Drug and chemical toxicology 2018;41(4):377-384
https://doi.org/10.1080/01480545.2018.1437173
.
2. Siblerud R, Mutter J, Moore E, Naumann J, Walach H. A hypothesis and evidence that mercury may be an etiological factor in Alzheimer’s disease. International Journal of Environmental Research and Public Health 2019;16(24):5152
https://doi.org/10.3390/ijerph16245152
.
3. Huang CF, Hsu CJ, Liu SH, Lin-Shiau SY. Neurotoxicological mechanism of methylmercury induced by low-dose and long-term exposure in mice: oxidative stress and down-regulated Na+/K+-ATPase involved. Toxicology letters 2008;176(3):188-197
https://doi.org/10.1016/j.toxlet.2007.11.004
.
4. Owoeye O, Arinola GO. A vegetable, Launaea taraxacifolia, mitigated mercuric chloride alteration of the microanatomy of rat brain. Journal of Dietary Supplements 2017;14(6):613-625
https://doi.org10.1080/19390211.2017.1288194
.
5. Jakaria M, Park SY, Haque ME, Karthivashan G, Kim IS, Ganesan P, et al. Neurotoxic agent-induced injury in neurodegenerative disease model: Focus on involvement of glutamate receptors. Frontiers in molecular neuroscience 2018;11: 307
https://doi.org/10.3389/fnmol.2018.00307
.
6. Rao MV, Purohit A, Patel T. Melatonin protection on mercury-exerted brain toxicity in the rat. Drug and Chemical Toxicology 2010;33(2):209-216
https://doi.org/10.3109/01480540903349258
.
7. Jha A, Saidullah B, Bubber P. A study on prooxidative and neurotoxic effects of mercury chloride in rats. EC Pharmacology and Toxicology 2019;7: 112-124.
8. Drew MR, Huckleberry KA. Modulation of aversive memory by adult hippocampal neurogenesis. Neurotherapeutics 2017;14(3):646-661
https://doi.org/10.1007/s13311-017-0528-9
.
9. Teixeira FB, Fernandes RM, Farias-Junior PM, Costa NM, Fernandes LM, Santana LN, et al. Evaluation of the effects of chronic intoxication with inorganic mercury on memory and motor control in rats. International journal of environmental research and public health 2014;11(9):9171-9185
https://doi.org/10.3390/ijerph110909171
.
10. Wu J, Cheng G, Lu Z, Wang M, Tian J, Bi Y. Effects of methyl mercury chloride on rat hippocampus structure. Biological trace element research 2016;171(1):124-130
https://doi.org/10.1007/s12011-015-0492-3
.
11. Teixeira FB, De Oliveira AC, Leão LK, Fagundes NC, Fernandes RM, Fernandes LM, et al. Exposure to inorganic mercury causes oxidative stress, cell death, and functional deficits in the motor cortex. Frontiers in molecular neuroscience 2018;11: 125
https://doi.org/10.3389/fnmol.2018.00125
.
12. Ayyathan DM, Chandrasekaran R, Thiagarajan K. Neuroprotective effect of Tagara, an Ayurvedic drug against methyl mercury induced oxidative stress using rat brain mitochondrial fractions. BMC Complementary and Alternative Medicine 2015;15(1):1-8
https://doi.org/10.1186/s12906-015-0793-2
.
13. Polash SA, Saha T, Hossain MS, Sarker SR. Investigation of the phytochemicals, antioxidant, and antimicrobial activity of the Andrographis paniculata leaf and stem extracts. Advances in Bioscience and Biotechnology 2017;8(05):149
https://doi.org/10.4236/abb.2017.85012
.
14. Khare CP.
Andrographis paniculata, Indian medicinal plants, an Illustrated Dictionary. New Delhi, India: Springer 2007;2: 49-50
https://doi.org/10.1007/978-0-387-70638-2_456
.
15. Okhuarobo A, Falodun JE, Erharuyi O, Imieje V, Falodun A, Langer P. Harnessing the medicinal properties of Andrographis paniculata for diseases and beyond: a review of its phytochemistry and pharmacology. Asian Pacific journal of tropical disease 2014;4(3):213-222
https://doi.org/10.1016/S2222-1808(14)60509-0
.
16. Sanjutha S, Subramanian S, Rani CI, Maheswari J. Integrated nutrient management in Andrographis paniculata
. Res J Agric Biol Sci 2008;4(2):141-145.
17. Verma H, Negi MS, Mahapatra BS, Shukla A, Paul J. Evaluation of an emerging medicinal crop Kalmegh [Andrographis paniculata (Burm F.) Wall. Ex. Nees] for commercial cultivation and pharmaceutical & industrial uses: A review. Journal of pharmacognosy and phytochemistry 2019;8(4):835-848.
18. Adedapo AA, Adeoye BO, Sofidiya MO, Oyagbemi AA. Antioxidant, antinociceptive and anti-inflammatory properties of the aqueous and ethanolic leaf extracts of Andrographis paniculata in some laboratory animals. Journal of Basic and Clinical Physiology and Pharmacology 2015;26(4):327-334
https://doi.org/10.1515/jbcpp-2014-0051
.
19. Zhang XF, Tan BK. Anti-diabetic property of ethanolic extract of Andrographis paniculata in streptozotocin-diabetic rats. Acta Pharmacologica Sinica 2000;21(12):1157-1164.
20. Jean-Barilla MS.
Andrographis paniculata: Can herbs fight common ailments, cancer, and chronic viral infections? A Keats Good Health Guide 1999;17-20.
21. Carlsen MH, Halvorsen BL, Holte K, Bøhn SK, Dragland S, Sampson L, et al. The total antioxidant content of more than 3100 foods, beverages, spices, herbs and supplements used worldwide. Nutrition journal 2010;9: 3
https://doi.org/10.1186/1475-2891-9-3
.
22. Association of Official Analytical Chemists (AOAC). Official methods of analysis XI edition: Association of official analytical chemists. 11th ed. Washington DC: The Association; 1970.
23. Salman MM, Kotb AM, Haridy MA, Hammad S. Hepato- and nephroprotective effects of bradykinin potentiating factor from scorpion (Buthus occitanus) venom on mercuric chloride-treated rats. EXCLI journal 2016;15: 807-816
https://doi.org/10.17179/excli2016-777
.
24. Niehaus WG, Samuelsson B. Formation of malonaldehyde from phospholipid arachidonate during microsomal lipid peroxidation. European Journal of Biochemistry 1968;6(1):126-30
https://doi.org/10.1111/j.1432-1033.1968.tb00428.x
.
25. Akanji MA, Adeyemi OS, Oguntoye SO, Sulyman F. Psidium guajava extract reduces trypanosomosis associated lipid peroxidation and raises glutathione concentrations in infected animals. EXCLI J 2009;8(1):148-154.
26. Aebi H, Wyss SR, Scherz B, Skvaril F. Heterogeneity of erythrocyte catalase II: isolation and characterization of normal and variant erythrocyte catalase and their subunits. European journal of biochemistry 1974;48(1):137-145
https://doi.org/10.1111/j.1432-1033.1974.tb03751.x
.
27. Fridovich I. Superoxide dismutases: an adaptation to a paramagnetic gas. Journal of Biological Chemistry 1989;264(14):7761-7764
https://doi.org/10.1016/S0021-9258(18)83102-7
.
28. Paglia DE, Valentine WN. Studies on the quantitative and qualitative characterization of erythrocyte glutathione peroxidase. The Journal of laboratory and clinical medicine 1967;70(1):158-169
https://doi.org/10.5555/uri:pii:0022214367900765
.
29. Bancroft JD, Layton C. The hematoxylin and eosin. In: Suvarna SK, Layton C, Bancroft JD, editors. Theory Practice of histological techniques. 7th ed. Ch. 10 and 11: Philadelphia: Churchill Livingstone of El Sevier; 2013. p. 179-220
http://dx.doi.org/10.1016/b978-0-7020-4226-3.00010-x
.
30. Yan Z, Liao H, Chen H, Deng S, Jia Y, Deng C, et al. Elevated intraocular pressure induces amyloid-β deposition and tauopathy in the lateral geniculate nucleus in a monkey model of glaucoma. Investigative ophthalmology & visual science 2017;58(12):5434-5443
https://doi.org/10.1167/iovs.17-22312
.
31. Esmaeili AH, Khavari-Nejad RA, Moghaddam AH, Chaichi MJ, Ebrahimzadeh MA. Effects of eriobotrya japonica (Lindl.) flower extracts on mercuric chloride-induced hepatotoxicity in rats. Chinese Science Bulletin 2012;57(30):3891-3897
https://doi.org/10.1007/s11434-012-5429-z
.
32. Raeeszadeh M, Moradi M, Ayar P, Akbari A. The antioxidant effect of Medicago sativa L.(alfalfa) ethanolic extract against mercury chloride (HgCl2) toxicity in rat liver and kidney: an in vitro and in vivo study. Evidence-Based Complementary and Alternative Medicine; 2021.
https://doi.org/10.1155/2021/8388002
.
33. Ahn CB, Song CH, Kim WH, Kim YK. Effects of Juglans sinensis dode extract and antioxidant on mercury chloride-induced acute renal failure in rabbits. Journal of ethnopharmacology 2002;82(1):45-49
https://doi.org/10.1016/S0378-8741(02)00124-1
.
34. Jaiswal N, Kumar D, Rizvi SI. Red onion extract (Allium cepa L.) supplementation improves redox balance in oxidatively stressed rats. Food Science and Human Wellness 2013;2(2):99-104
https://doi.org/10.1016/j.fshw.2013.05.003
.
35. Khaki A, Fathiazad F, Nouri M. Effects of watermelon seed extract (Citrullus vulgaris) on spermatogenesis in rat. International Journal of Women’s Health and Reproduction Sciences 2013;1(3):99-104.
36. Mieiro CL, Pereira ME, Duarte AC, Pacheco M. Brain as a critical target of mercury in environmentally exposed fish (Dicentrarchus labrax)-bioaccumulation and oxidative stress profiles. Aquatic Toxicology 2011;103(3–4):233-240
https://doi.org/10.1016/j.aquatox.2011.03.006
.
37. Branco V, Canário J, Lu J, Holmgren A, Carvalho C. Mercury and selenium interaction in vivo: effects on thioredoxin reductase and glutathione peroxidase. Free Radical Biology and Medicine 2012;52(4):781-793
https://doi.org/10.1016/j.freeradbiomed.2011.12.002
.
38. Vijayaprakash S, Langeswaran K, Kumar SG, Revathy R, Balasubramanian MP. Nephro-protective significance of kaempferol on mercuric chloride induced toxicity in Wistar albino rats. Biomedicine & aging pathology 2013;3(3):119-124
https://doi.org/10.1016/j.biomag.2013.05.004
.
39. Ishola AA, Oyinloye BE, Ajiboye BO, Kappo AP. Molecular docking studies of flavonoids from Andrographis paniculata as potential acetylcholinesterase, butyrylcholinesterase and monoamine oxidase inhibitors towards the treatment of neurodegenerative diseases. Biointerface Res. Appl. Chem 2021;11: 9871-9879
https://doi.org/10.33263/BRIAC113.98719879
.
40. Li B, Jiang T, Liu H, Miao Z, Fang D, Zheng L, et al. Andrographolide protects chondrocytes from oxidative stress injury by activation of the Keap1–Nrf2–Are signaling pathway. Journal of cellular physiology 2018;234(1):561-571
https://doi.org/10.1002/jcp.26769
.
41. Tan WD, Liao W, Peh HY, Vila M, Dong J, Shen HM, et al. Andrographolide simultaneously augments Nrf2 antioxidant defense and facilitates autophagic flux blockade in cigarette smoke-exposed human bronchial epithelial cells. Toxicology and Applied Pharmacology 2018;360: 120-130
https://doi.org/10.1016/j.taap.2018.10.005
.
42. Mussard E, Cesaro A, Lespessailles E, Legrain B, Berteina-Raboin S, Toumi H. Andrographolide, a natural antioxidant: an update. Antioxidants (Basel) 2019;8(12):571
https://doi.org/10.3390/antiox8120571
.
43. Aragão WAB, Teixeira FB, Fagundes NCF, Fernandes RM, Fernandes LMP, da Silva MCF, et al. Hippocampal dysfunction provoked by mercury chloride exposure: evaluation of cognitive impairment, oxidative stress, tissue injury and nature of cell death. Oxidative medicine and cellular longevity; 2018.
https://doi.org/10.1155/2018/7878050
.
44. Weis JS, Smith G, Zhou T, Santiago-Bass C, Weis P. Effects of contaminants on behavior: biochemical mechanisms and ecological consequences: killifish from a contaminated site are slow to capture prey and escape predators; altered neurotransmitters and thyroid may be responsible for this behavior, which may produce population changes in the fish and their major prey, the grass shrimp. Bioscience 2001;51(3):209-217
https://doi.org/10.1641/0006-3568(2001)051[0209:EOCOBB]2.0.CO;2
.
45. Jha R, Rizvi SI. Age-dependent decline in erythrocyte acetylcholinesterase activity: correlation with oxidative stress. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 2009;153(3):195-198
https://doi.org/10.5507/bp.2009.032
.
46. Molochkina EM, Zorina OM, Fatkullina LD, Goloschapov AN, Burlakova EB. H2O2 modifies membrane structure and activity of acetylcholine esterase. Chemico-Biological Interactions 2005;157: 401-404
https://doi.org/10.1016/j.cbi.2005.10.075
.
47. Abu-Taweel GM. Neurobehavioral protective properties of curcumin against the mercury chloride treated mice offspring. Saudi journal of biological sciences 2019;26(4):736-743
https://doi.org/10.1016/j.sjbs.2018.10.016
.
48. Kim MH, Min JS, Lee JY, Chae U, Yang EJ, Song KS, et al. Oleuropein isolated from Fraxinus rhynchophylla inhibits glutamate-induced neuronal cell death by attenuating mitochondrial dysfunction. Nutritional neuroscience 2018;21(7):520-528
https://doi.org/10.1080/1028415X.2017.1317449
.
49. Kritis AA, Stamoula EG, Paniskaki KA, Vavilis TD. Researching glutamate-induced cytotoxicity in different cell lines: a comparative/collective analysis/study. Frontiers in Cellular Neuroscience 2015;9: 91
https://doi.org/10.3389/fncel.2015.00091
.
50. Albrecht J, Matyja E. Glutamate: a potential mediator of inorganic mercury neurotoxicity. Metabolic Brain Disease 1996;11(2):175-184
https://doi.org/10.1007/BF02069504
.
51. Phan CW, David P, Naidu M, Wong KH, Sabaratnam V. Therapeutic potential of culinary-medicinal mushrooms for the management of neurodegenerative diseases: diversity, metabolite, and mechanism. Critical Reviews in Biotechnology 2015;35(3):355-368
https://doi.org/10.3109/07388551.2014.887649
.
52. Owoeye O, Farombi EO. Tomato pomace protects against mercuric chloride-induced neurodegeneration and motor abnormality in adult rat. International Journal of Biological and Chemical Sciences 2015;9(3):1142-1153
https://doi.org/10.4314/ijbcs.v9i3.1
.
53. Uma C, Poornima K, Surya S, Ravikumar G, Gopalakrishnan VK. Nephroprotective Effect of Ethanolic Extract of Tabernaemontana Coronaria in Mercuric Chloride InducedRenal Damage in Wistar Albino Rats. International Journal of Chemical Engineering and Applications 2012;3(4):269.
54. Bernhoft RA. Mercury Toxicity and Treatment: A review of the literature. Journal of Environmental and Public Health 2012;10:
https://doi.org/10.1155/2012/460508
.
55. Verma N, Vinayak M. Antioxidant action of Andrographis paniculata on lymphoma. Molecular biology reports 2008;35(4):535-540
https://doi.org/10.1007/s11033-007-9119-x
.
Figure 1Bar charts of Oxidative stress parameters ((a) SOD, (b) CAT, (c) GPx and (d) MDA) after 4 weeks of the experiment. Data were analyzed using one way ANOVA, followed with Tukey post hoc test. *p<0.033; ** p< 0.002; *** p< 0.0001 indicates a significant difference when compared to normal control; #p<0.03; ## p< 0.002; ### p< 0.0001, indicates a significant difference when compared to HgCl2 control group. 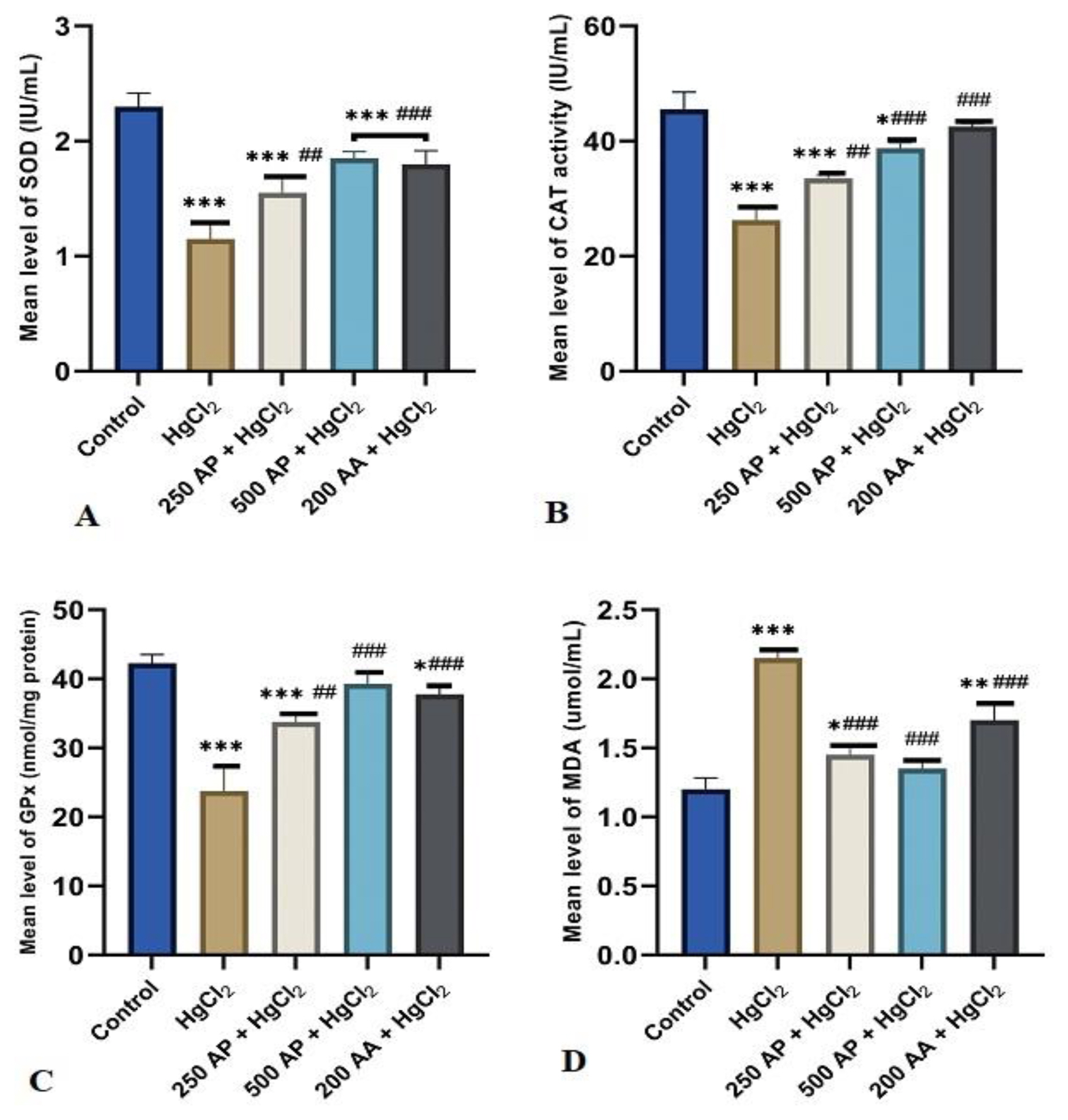
Figure 2Bar chats of the Neuronal Assay ((a) AChE activity, (b) Dopamine, and (c) Glutamate after 4 weeks of the experiment. Data were analyzed using one way ANOVA, followed with Tukey post hoc test. *p<0.033; ** p< 0.002; *** p<0.0001 indicates a significant difference when compared to normal control; #p<0.03; ## p<0.002; ### p< 0.0001, indicates a significant difference when compared to HgCl2 control group. 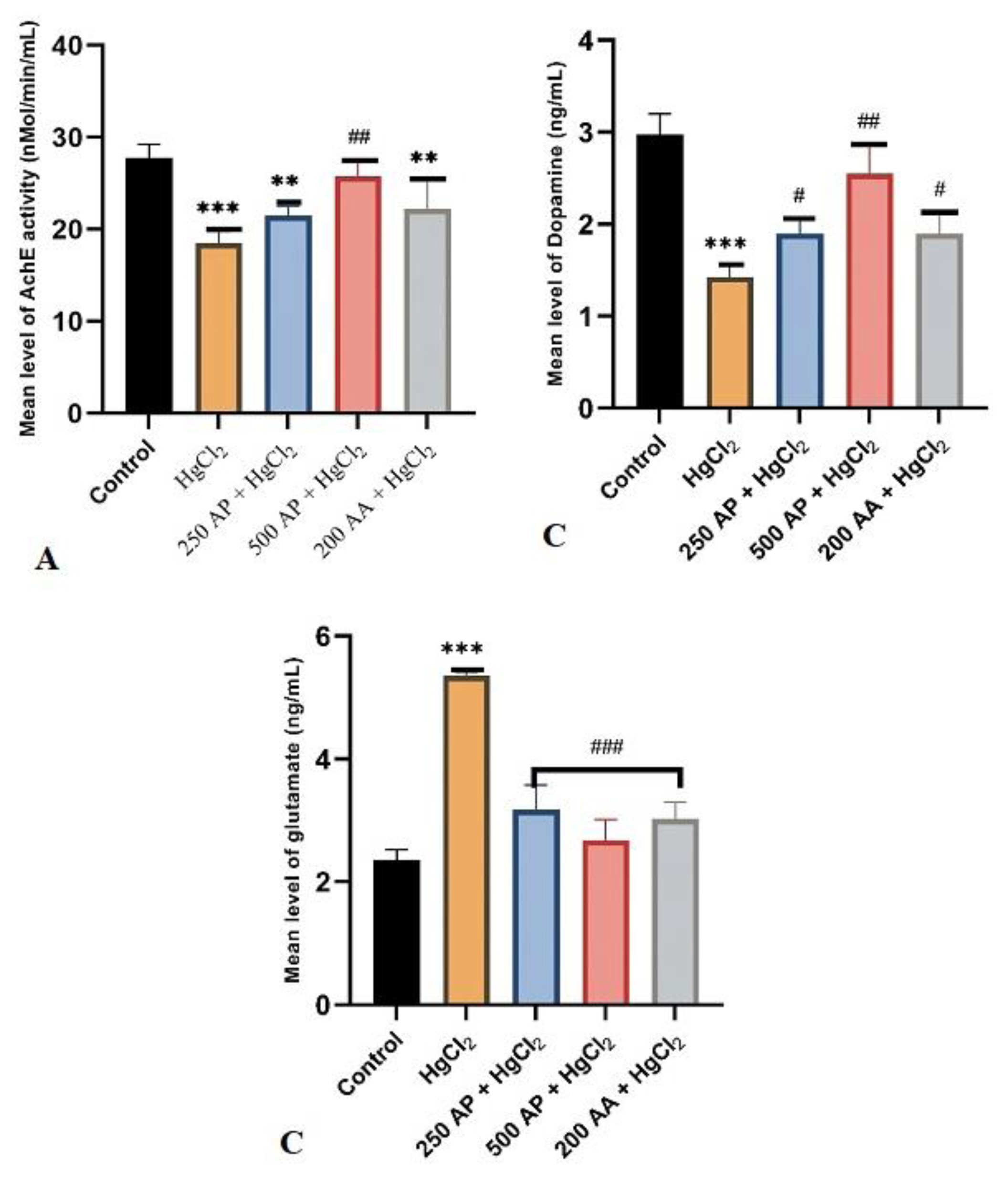
Figure 3Composite photomicrographs of hippocampus of control (A) showing compact layers of small pyramidal cells of CA1 region, most with vesicular nuclei; the pyramidal cell-layer neurons (blue arrow) of CA3 are uniform in size and equally distributed. Each neuron features a large nucleolus and a rounded central vesicular nucleus in both CA1 and CA3 (blue arrow). HgCl2 treated micrograph (B) most neurons have shrunken nuclei and vacuolated cytoplasm, some have pyknotic nuclei or karyolysis (blue arrow) at CA1 region. There are areas that are devoid of pyramidal neurons, apoptosis is visible in some CA3 big pyramidal cells, as well as clumping of neuronal fibrils (blue arrow). Extract 250/500 mg/kg+0.5 mg/kg HgCl2 (C and D) showed preservation of pyramidal cells except for deepest layer with clumping of neuronal fibrils at CA1 and CA3 region. Ascorbic Acid treated group (E) showed preservation of pyramidal cells but with mild clumping and disorganization of granular and pyramidal cells with dilated vessels (v) and normal glial cells (*) in molecular layer at both CA1 CA3 region (H & E x400). 
Figure 4Composite photomicrograph of CA1 and CA3 hippocampal subfields of the brain of rats treated with HgCl2, AP+HgCl2 and AA+HgCl2 showing normal pyramidal cells in A and D, mild distortion in C and E and degeneration and neuronal loss in B of both CA1 and CA3. Bielschowsky x 400. 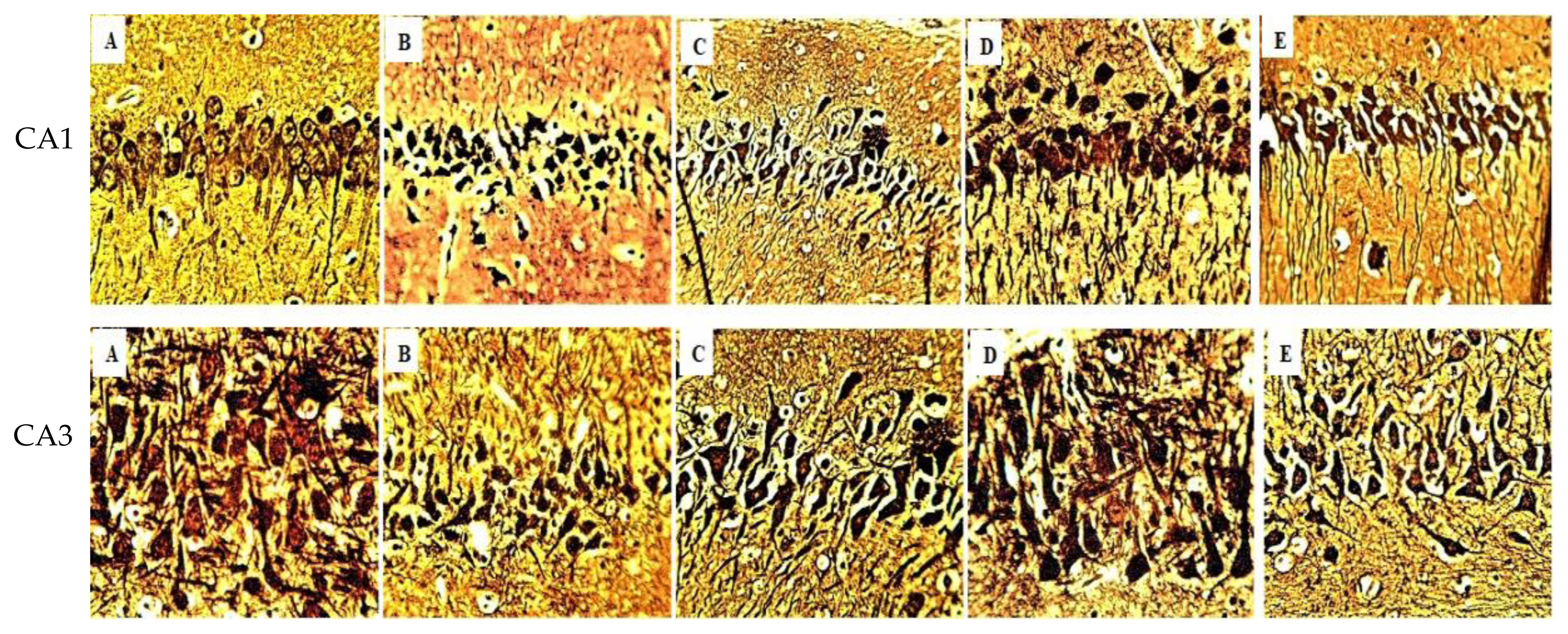
Figure 5Representative photomicrographs of brain sections of rats (Cerebellar cortices) stained by H&E. Control (A) showing normal orientation of the Molecular layer, Granular layer, and Purkinje layer with normal Purkinje cells (arrow), HgCl2 treated micrograph (B) showing normal Granular layer, normal Molecular Layer and degeneration of purkinje cells and it’s layer (arrow), Extract 250/Ascorbic acid 200 mg/kg+0.5 mg/kg HgCl2 (C&E) showed showing densely packed Granular Layer, slight ballooning degenerated purkinje cells and normal Molecular layer, Extract 250/500 mg/kg+0.5 mg/kg HgCl2 showing normal orientation of the Molecular layer, Granular layer, and Purkinje layer with normal Purkinje cells (H & E x400; Bielschowsky x 400). 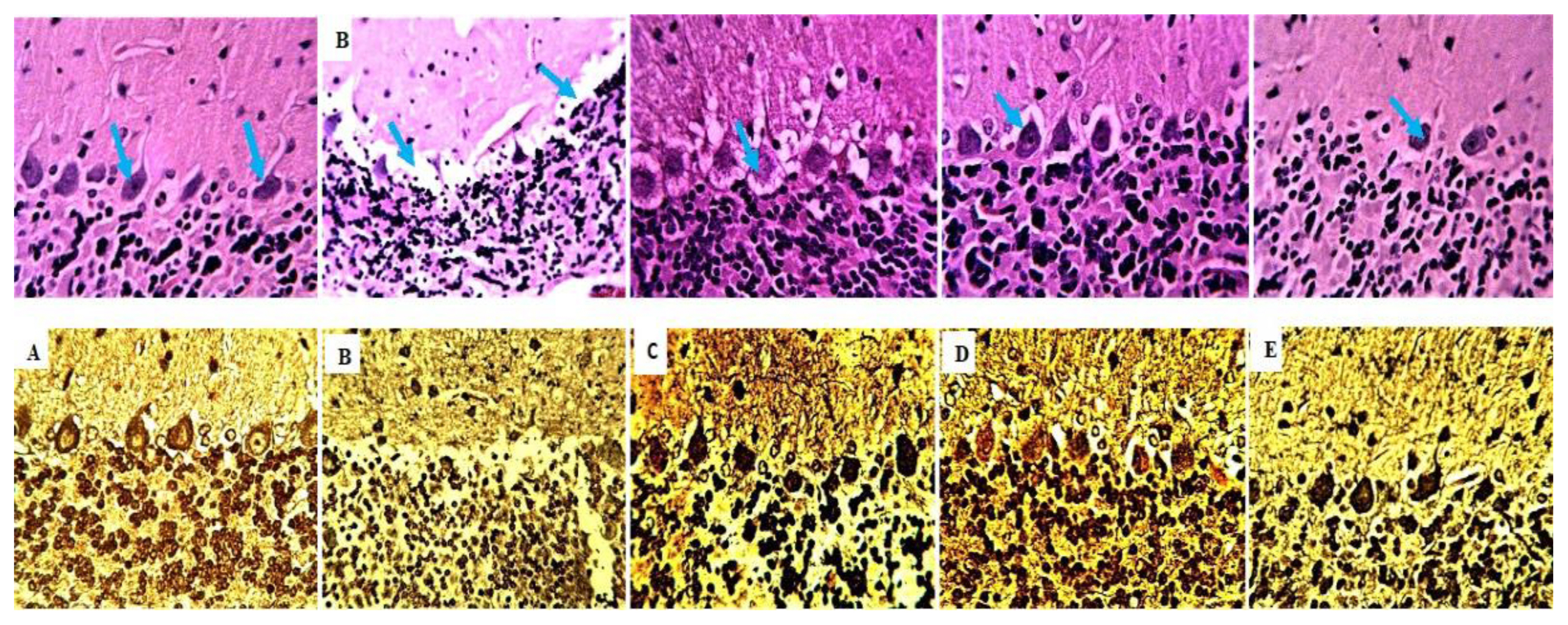
Table 1A summary of the experimental design. Table 2Effect of A. paniculata and mercury chloride treatments on body weight.
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||